Organelle & Cell & Tissue Targeting Liposomes Formulation and Development
Introduction of Targeting Liposomes
Over the past few decades, nanomedicine, particularly liposomal drug delivery, has attracted extensive attention. Attributes including low batch-to-batch variability, ease of synthesis, scalability, and biocompatibility have offered liposomes substantial advantages over many other nanoparticular drug delivery system.
One of the most outstanding traits of liposomes would be their flexibility for surface modification to enhance the selective targeting of cells/organs. Specific targeting of tissues and cells can either be passive, for long circulating liposomes, or active, for liposomes conjugated to ligands with specific affinity for receptors within a tissue, cell or intracellular target.1
In the oncology field, passive targeting is mostly associated with the Enhanced Permeability and Retention effect (EPR), as there are obvious evidence proving that the preferential accumulation of liposomes of a specific size range of 100 to 200nm into the tumor interstitial space is specially owing to the EPR effect.2 Figure 1 is taken from reference 3 which illustrate the mechanism. However, the passive targeting effect is strictly limited to some EPR-featured solid tumors that are larger than approximately 4.6 mm in diameter, while lots of factors could interfere such a phenomenon.4 Herein, active targeting on cancer therapy is imperative.
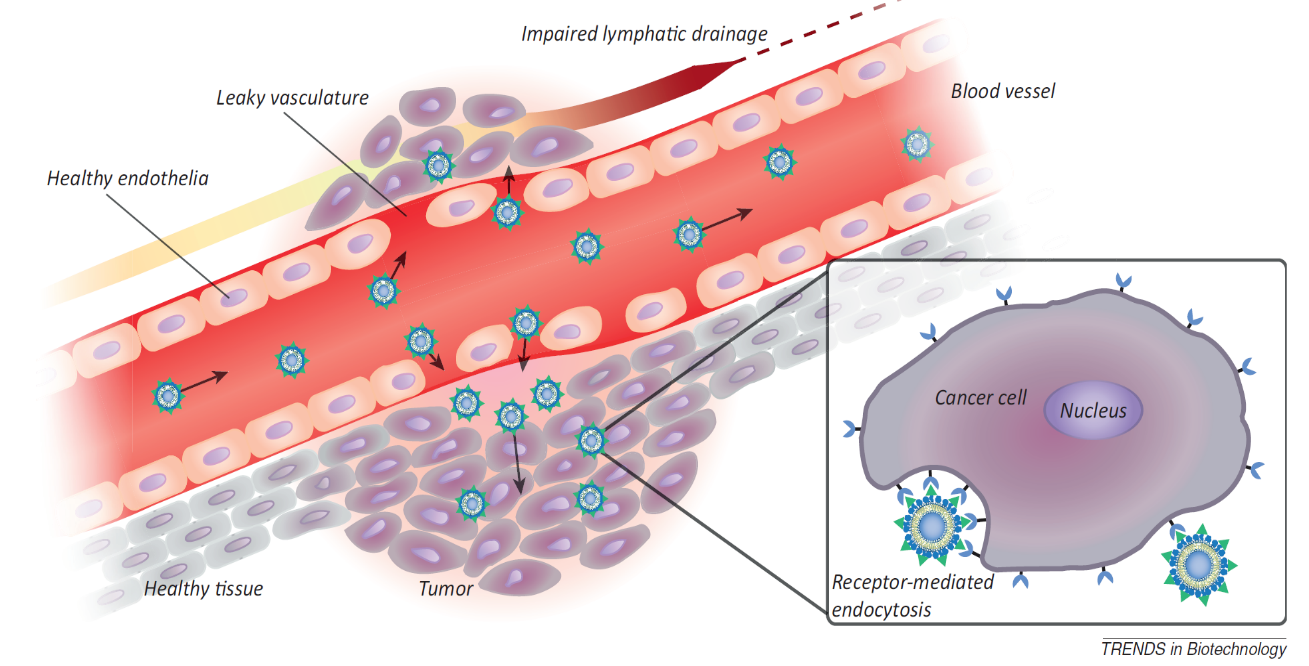
Figure 1. Passive targeting of nanoparticles to tumors through the enhanced permeability and retention (EPR) effect. Angiogenic vessels in rapidly growing tumors are abnormally constructed with large vascular fenestrae and impaired lymphatic drainage. As a result, particles <200 nm preferentially accumulate in the tumor interstitium. Post-extravasation, intracellular uptake of ligand-targeted liposomes is facilitated by receptor-mediated endocytosis.
Active targeting is achieved by specific modification of liposomal surface with a targeting ligand, which can contribute to their accumulation at the desired site or intracellular delivery to cell of interest. Ideal targets are expressed homogenously and at high levels by the tumor cell population, have negligible or low expression in healthy tissues, and are surface expressed to allow for liposome binding.5 This is the main reason why the concept of active targeting is mainly brought up in oncology other than other fields, as most cancer cells origin from abnormal regulation of genes, accompanied with the overexpression of certain proteins. For example, human epidermal growth factor receptor 2 (HER2) is overexpressed at levels up to 1,000-fold higher than normal in ~25% of breast cancer cases, and ligand-targeted liposomes (LTLs) against HER2 have shown successful preclinical outcomes.6
A number of targeting ligands have been proposed for development of targeted liposomal formulations. These include proteins (antibodies or antibody fragments), nucleic acids (aptamers) and other receptor ligands (peptides, carbohydrates, and vitamins). Antibody or antibody fragments (Fab or scFv) are among the most frequently used ligands for targeted therapies owing to their high affinity and specificity for the target receptor. Although early studies focused on the use of whole antibodies, it is now recognized that antibody fragments have reduced immunogenicity and improved pharmacokinetics profiles and are therefore preferred in the clinic.4 Peptides and peptidomimetics are also emerging as favored targeting ligands owing to ease of preparation, lower cost, lower antigenicity, decreased opsonization, and increased resistance to enzymatic degradation.7 In particular, advancements in phage display libraries have enabled the identification of numerous novel, site-specific peptides and peptidomimetics for potential use as targeting ligands. Table 1 is taken from reference 3 listing out various applicable ligands for active targeting.
Active targeting has led subcellular targeting accessible, particularly for vital disease-related locations such the nucleus and mitochondria. Many special moieties have been applied to achieve successful organelle targeting including Nuclear Localization Signal (NLS) that shuttle the cargo specifically to nucleus, and mitochondria targeting sequence (MTS) motifs termed KLA-DMA, the formulation of which contribute to efficient lung cancer cell (A549) targeting.8
Although liposomes have already made their transition into the clinic, the current clinically available liposome-based therapies do not exhibit active targeting at the cellular level and therefore do not harness the full potential that nanotechnology can provide. LTLs have demonstrated improved efficacy over passively targeted equivalents through enhanced tumor targeting and intracellular uptake and deserve future investigations.
Key Targeting Liposomes Services We Can Offer:
-
Design and screen the suitable organelle/cell/tissue targeting modifications for targeting delivery
-
Optimized bioconjugation strategies with improved consistency and specificity
-
Optimize the liposomal cargos for your R&D purposes
-
Lipid library development for active-delivery studies
-
Targeting activity analysis and evaluation
Key Targeting Liposomes Features:
-
Passive targeting by size & active targeting by surface modification
-
3 Main methods to achieve surface modification (figure 2 is taken from reference 9):
-
Binding the desired targeting ligand to a lipid prior to mixing them with other lipid components during liposome preparation;
-
Liposome are functionalized with the required targeting ligand immediately after preparation;
-
Postinsertion of the functionalized lipid in preformed liposomes
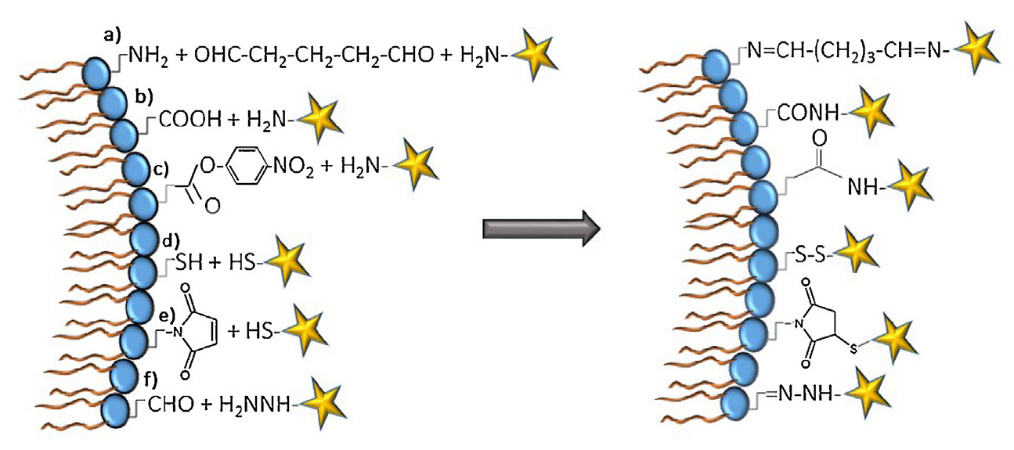
Figure 2. Classical methods for coupling ligands. Schematic representation of a cross section of a liposome bilayer containing functional groups to illustrate (a) crosslinkingof primary amines by glutaraldehyde, (b) carbonyl-amine bond formation, (c) amide bond formation by the reaction of para-nitrophenylcarbonyl with primary amine, (d)disulfide bond formation, (e) thioester bond formation by the maleimidethiol addition reaction, and (f) hydrazone bond formation. Coupling ligands are represented by stars.9
Key Targeting Liposomes Benefits
-
Low batch-to-batch variability
-
Ease of synthesis
-
Scalability
-
Biocompatibility
Targeting Liposomes Applications
-
Great improvement in cancer therapy
-
Can be precise diagnostic/imaging tools
References:
1. Lehner R, Wang X, Marsch S, Hunziker P. Intelligent nanomaterials for medicine: carrier platforms and targeting strategies in the context of clinical application. Nanomedicine. 2013 Aug;9(6):742-57. doi: 10.1016/j.nano.2013.01.012. Epub 2013 Feb 19. PMID: 23434677.
2. Allen TM, Cullis PR. Liposomal drug delivery systems: from concept to clinical applications. Adv Drug Deliv Rev. 2013 Jan;65(1):36-48. doi: 10.1016/j.addr.2012.09.037. Epub 2012 Oct 1. PMID: 23036225.
3. Noble GT, Stefanick JF, Ashley JD, Kiziltepe T, Bilgicer B. Ligand-targeted liposome design: challenges and fundamental considerations. Trends Biotechnol. 2014 Jan;32(1):32-45. doi: 10.1016/j.tibtech.2013.09.007. Epub 2013 Nov 6. PMID: 24210498.
4. Sawant RR, Torchilin VP. Challenges in development of targeted liposomal therapeutics. AAPS J. 2012 Jun;14(2):303-15. doi: 10.1208/s12248-012-9330-0. Epub 2012 Mar 14. PMID: 22415612; PMCID: PMC3326155.
5. Sapra P, Allen TM. Ligand-targeted liposomal anticancer drugs. Prog Lipid Res. 2003 Sep;42(5):439-62. doi: 10.1016/s0163-7827(03)00032-8. PMID: 12814645.
6. Stefanick JF, Ashley JD, Kiziltepe T, Bilgicer B. A systematic analysis of peptide linker length and liposomal polyethylene glycol coating on cellular uptake of peptide-targeted liposomes. ACS Nano. 2013 Apr 23;7(4):2935-47. doi: 10.1021/nn305663e. Epub 2013 Mar 5. PMID: 23421406.
7. Ruoslahti E. Peptides as targeting elements and tissue penetration devices for nanoparticles. Adv Mater. 2012 Jul 24;24(28):3747-56. doi: 10.1002/adma.201200454. Epub 2012 May 2. PMID: 22550056; PMCID: PMC3947925.
8. Jiang L, Li L, He X, Yi Q, He B, Cao J, Pan W, Gu Z. Overcoming drug-resistant lung cancer by paclitaxel loaded dual-functional liposomes with mitochondria targeting and pH-response. Biomaterials. 2015 Jun;52:126-39. doi: 10.1016/j.biomaterials.2015.02.004. Epub 2015 Feb 24. PMID: 25818419.
9. Noble GT, Stefanick JF, Ashley JD, Kiziltepe T, Bilgicer B. Ligand-targeted liposome design: challenges and fundamental considerations. Trends Biotechnol. 2014 Jan;32(1):32-45. doi: 10.1016/j.tibtech.2013.09.007. Epub 2013 Nov 6. PMID: 24210498.



