What are Soluble Microneedle Patches?
Introduction
Delivering drugs through the skin has long been an attractive goal in pharmaceutical science. Compared with injections, transdermal delivery can improve patient comfort, reduce medical waste, and enable self-administration without professional assistance. However, the outermost layer of the skin—the stratum corneum—forms a highly effective barrier that prevents most drugs from entering the body efficiently. Overcoming this barrier while maintaining safety and convenience has been a major challenge in drug delivery research.
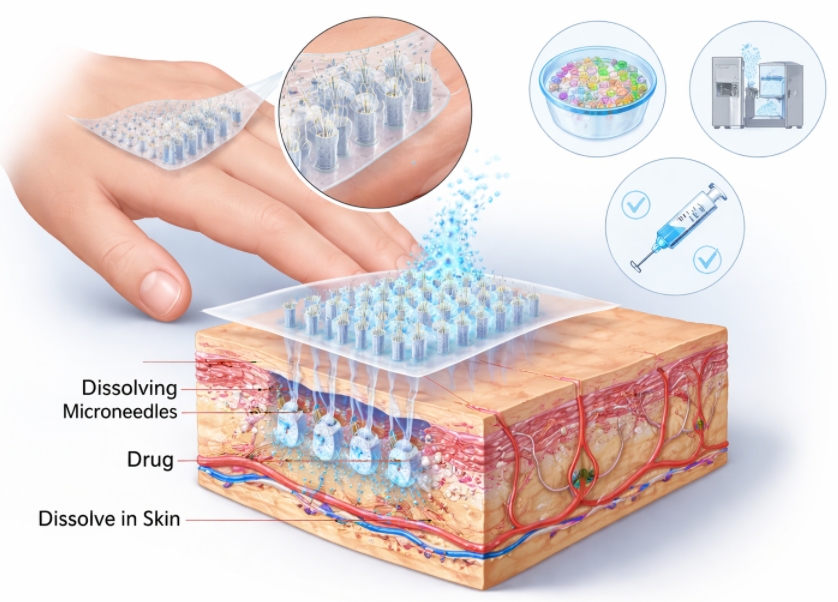
Soluble microneedle patches have emerged as a promising technology designed to address this challenge. These patches contain arrays of microscopic needles made from water-soluble and biocompatible materials. When applied to the skin, the microneedles penetrate the outer barrier layer and dissolve within the skin tissue, releasing the drug payload directly into the targeted region. Because the needles dissolve completely, the system eliminates concerns about needle disposal and reduces the risk of accidental injury.
In recent years, soluble microneedle patches have attracted increasing attention from researchers, pharmaceutical developers, and clinicians. Continuous progress in material science, microfabrication, and pharmaceutical formulation has significantly improved the performance of these systems. Modern research now focuses not only on demonstrating the feasibility of microneedle delivery, but also on optimizing drug release speed, stability, loading capacity, and clinical applicability.
Understanding the Structure and Mechanism of Soluble Microneedles
A soluble microneedle patch is typically composed of a flexible backing layer and a dense array of microscopic needles arranged on its surface. These needles are usually a few hundred micrometers long, which allows them to penetrate the stratum corneum without reaching deeper nerve endings or blood vessels. As a result, the application process is generally painless or causes only minimal discomfort.
The microneedles themselves are fabricated from biodegradable and water-soluble polymers such as polyvinylpyrrolidone, hyaluronic acid, or other biocompatible materials. Drugs are incorporated into the polymer matrix during fabrication. Once the patch is applied to the skin, the microneedles pierce the outer barrier and begin to absorb interstitial fluid from surrounding tissues.
As the microneedle matrix hydrates, it gradually dissolves, releasing the encapsulated drug molecules directly into the epidermal or dermal layers of the skin. These layers contain dense networks of capillaries and immune cells, which allow drugs to enter systemic circulation or act locally within the tissue. Because the microneedles dissolve completely after administration, no solid sharps remain in the skin or on the patch.
This unique mechanism offers several advantages. It improves drug delivery efficiency, reduces discomfort compared with injections, and simplifies administration for patients who may need frequent treatments. These characteristics have positioned soluble microneedles as a powerful platform for future transdermal therapies.
Rapid Dissolution Technologies for Faster Drug Delivery
One of the earliest challenges encountered in dissolving microneedle systems was the relatively slow drug release process. Traditional designs sometimes required several minutes for the microneedles to fully dissolve after insertion. In clinical settings where rapid drug action is required, such delays can limit practical usability.
Recent technological advances have focused on accelerating microneedle dissolution. Researchers have discovered that modifying the material composition of the microneedle matrix can significantly improve hydration speed and structural breakdown after insertion into the skin.
For example, incorporating highly water-soluble components such as sodium bicarbonate into polymer matrices like polyvinylpyrrolidone has proven effective in accelerating dissolution kinetics. When the microneedle enters the skin environment, these additives promote rapid fluid penetration into the polymer structure, leading to faster needle degradation and drug release.
With optimized formulations, modern microneedle patches can deliver therapeutic compounds within seconds. This rapid dissolution enables almost immediate drug availability in the skin, which is particularly valuable for medications that require fast onset of action, such as local anesthetics. In practical terms, such systems may dramatically shorten waiting times compared with traditional topical formulations that often require extended periods before producing noticeable effects.
Manufacturing Innovation Through Freeze-Drying Technology
Another important area of development involves improving the manufacturing process of soluble microneedles. Conventional fabrication methods typically rely on mold casting followed by drying under controlled conditions. While effective, these processes can be sensitive to environmental factors such as humidity and temperature, which may introduce variability between batches.
To address these challenges, researchers have introduced freeze-drying, also known as lyophilization, into microneedle fabrication. Freeze-drying is widely used in pharmaceutical manufacturing because it preserves the stability of sensitive biological compounds while producing highly porous structures.
During the freeze-drying process, water is removed from frozen materials through sublimation. This creates microscopic pores throughout the microneedle matrix. The porous structure improves water absorption once the microneedles are inserted into the skin, allowing interstitial fluid to penetrate the structure more quickly.
As a result, freeze-dried microneedles often dissolve significantly faster than those produced through traditional drying methods. The porous architecture also improves drug stability during storage, particularly for sensitive biomolecules such as proteins and peptides. These improvements can help maintain the biological activity of therapeutic compounds even under elevated storage temperatures.
Precision Drug Localization for Dermatological Therapies
Soluble microneedle patches are particularly well suited for dermatological applications where drugs need to be delivered directly to specific skin layers. Conditions such as hypertrophic scars and keloids involve abnormal cellular activity in the dermis, making targeted drug delivery essential for effective treatment.
To improve therapeutic efficiency, researchers have developed microneedle systems with specialized structural designs that concentrate drugs at the needle tips. This approach ensures that the majority of the drug payload is deposited precisely in the tissue region where it is most needed.
One effective strategy involves creating dual-layer microneedles. In these systems, the drug is concentrated in the tip portion while the base layer primarily provides structural support. When the patch penetrates the skin, the drug-rich tips dissolve within the dermal layer, delivering a concentrated dose directly to the target site.
Such localized delivery strategies can significantly enhance treatment outcomes while minimizing systemic exposure. In experimental scar models, tip-loaded dissolving microneedles have shown strong potential for suppressing excessive fibroblast activity and reducing collagen accumulation—two major factors responsible for pathological scar formation.
Advancing Peptide and Protein Drug Delivery
Large biomolecules such as peptides and proteins represent some of the most promising modern therapeutics. However, delivering these molecules through the skin presents unique challenges due to their size and sensitivity. Additionally, microneedle structures offer limited internal volume for drug loading, which historically restricted their ability to deliver sufficient doses of macromolecular drugs.
Recent design innovations have begun to overcome these limitations. One strategy involves concentrating purified drug compounds directly within the microneedle tips rather than distributing them evenly throughout the polymer matrix. This “pure drug tip” approach allows a significantly higher drug payload to be incorporated into a relatively small patch area.
Using this strategy, researchers have successfully developed microneedle systems capable of delivering therapeutic peptide drugs used in metabolic disease treatment. These systems can load milligram-scale quantities of peptide compounds within patches smaller than one square centimeter.
Preclinical studies have demonstrated encouraging pharmacokinetic profiles, with efficient drug absorption and bioavailability approaching that of traditional subcutaneous injections. Importantly, these patches typically cause only mild and temporary skin reactions, suggesting good tolerability for repeated use.
Future Trends in Soluble Microneedle Research
The field of soluble microneedle technology is evolving rapidly, and the focus of research is shifting from basic feasibility toward performance optimization and clinical translation. Scientists are increasingly exploring how to make microneedle systems faster, more stable, and capable of delivering larger and more complex drugs.
Material engineering continues to play a central role. By adjusting polymer composition and incorporating dissolution-promoting additives, researchers are achieving faster drug release profiles that better match clinical requirements. At the same time, manufacturing innovations such as freeze-drying are improving product consistency and extending shelf life.
Another important direction is expanding the range of therapeutic applications. While early studies primarily focused on vaccine delivery, newer research is exploring microneedle-based treatments for pain management, metabolic diseases, dermatological conditions, and biologic drug administration.
As these technologies continue to mature, soluble microneedle patches may transform the way many medicines are delivered. Their ability to combine painless administration, precise drug targeting, and simplified dosing makes them a compelling solution for both patients and healthcare providers. With ongoing advances in materials, manufacturing, and drug formulation, soluble microneedles are increasingly positioned to play a significant role in the future of drug delivery.
Related Services
Soluble Microneedle Patches for DNA Vaccines-Based Drug Delivery System
Soluble Microneedle Patches for Peptide Drugs-Based Drug Delivery System
Soluble Microneedle Patches for Poorly Soluble Drugs-Based Drug Delivery System
Soluble Microneedle Patches for Protein Vaccines-Based Drug Delivery System
Soluble Microneedle Patches for Acne and Hyperpigmentation Treatment-Based Drug Delivery System
